A stroke occurs when blood flow to a specific region of the brain is obstructed. There is a rapid loss of brain function lasting twenty-four hours or more. Most strokes occur from a thrombosis (blood clot) that in turn causes ischemia. A small percentage (10%) of strokes occurs when there is a rupture in a vessel and blood leaks into the brain tissue and/or cerebral spinal fluid. Risk factors for stroke include hypertension, hyperlipidemia, smoking, diabetes, CAD, atrial fibrillation, poor diet, sedentary lifestyle, and alcoholism.
The lack of blood flow to the brain during a stroke causes both primary neural cell death and secondary impairments. The degree of neurological deficit depends on the size and location of the lesion as well as the speed with which it occurs. Slow developing lesions will tend to form collateral blood flow and have less impairment associated with it.
There are a number of problems individuals may experience after a stroke. Paralysis is one the most common problems. It is usually on one side of the body, opposite the side of the lesion. Paralysis may affect the face, arm, trunk or leg. Or, it may affect the entire side of the body. Damage to the cerebellum can affect coordinated movements, balance, walking and posture. People may experience sensory disturbances and lose the ability to feel touch, pain, temperature or position. A quarter of people who have had a stroke develop language impairments involving the ability to speak and write and/or to understand speech or written language. Individuals may also have cognitive dysfunction, short attention spans, and memory loss. Many stroke survivors also suffer emotional disturbances including increased fear, anxiety, frustration, aggression and sadness.
Acquired traumatic brain injury (TBI) can result from a blow or jolt to the head. After TBI, impairments in cognitive reasoning, language, memory, attention, reasoning, information processing, and speech may occur. Falls and motor vehicle accidents are the most common cause of TBI’s and typically occur between ages 0-4 years, 15-19 years and then later in life (>75 years).
When an individual sustains a blow to the head, the primary damage occurs at the point of impact followed by the opposite side as the brain bounces off the cranium. Diffuse axonal injury occurs with rapid acceleration and deceleration of the brain in the cranium. Secondary injury occurs with the subsequent edema compressing the uninvolved surrounding tissue.
Generally, people recovering from stroke and TBI have lower functional capacities than their pre-injury state. Disturbances in motor function may contribute to an impaired cardiac response in both stroke and TBI. As such, these individuals fatigue quickly, are less mobile and have increased energy expenditure during ADL’s. Exercise training has been shown to increase maximum oxygen consumption, workload response and decrease resting heart rate. Exercise following stroke has demonstrated an increase in walking speed, decreased ambulation assistance and improved functional mobility.
Stroke and TBI survivors are commonly on a variety of medications to combat seizures, depression, hypertonia, cognitive deficits. The effect of some medications may cause post-exercise hypotension and blunted heart rate response. As such, it is important to consider medications and the potential impact on designing an exercise program.
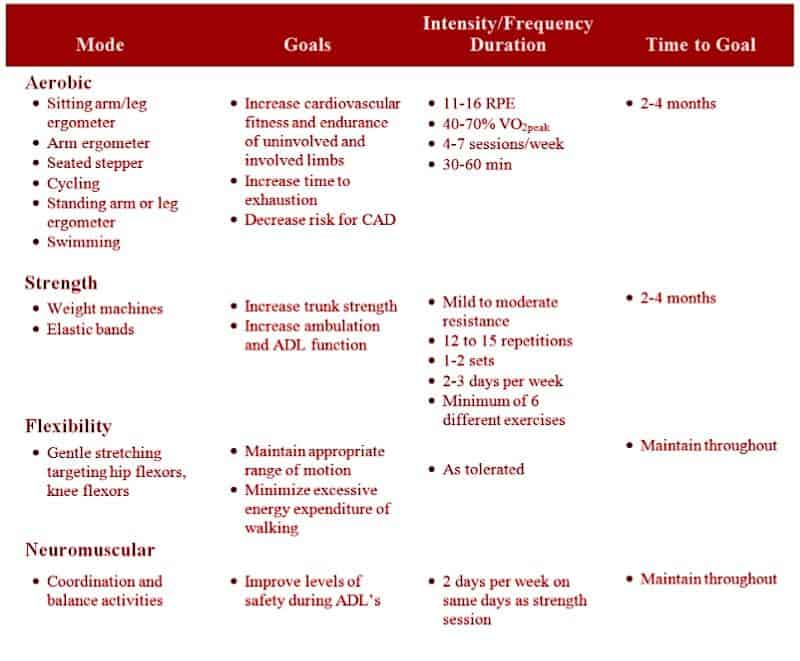
Endurance training for stroke survivors should entail a three-tier approach. Initially, the goal is to return to maximum potential function. The second tier is to reduce the risk of additional stroke and cardiovascular disease with appropriate diet modifications, weight loss, managing blood pressure and decreasing cholesterol. The goal of the third tier is to improve aerobic fitness. Various modes should be available pending the accommodation of equipment to meets a client’s motor impairments. The frequency of exercise sessions should be three to five days per week. Intensity should start as low as 40% of VO2peak with intermittent segments 5-10 minutes long, increasing to continuous exercise up to 60 minutes. Incorporating resistance training two to three days per week has been shown to be safe and effective for this population. Exercise should address any muscular weakness associated with a lack of function.
There are some additional considerations the must be addressed when working with this population. Individuals who have had a TBI or stroke may have behavioral factors such as impulsivity, lack of judgment, misunderstanding of directions and significant balance and motor control problems that will require direct and close supervision during exercise sessions. It may be more conducive to schedule certain client’s at a quieter time or in a less distracting area. Depression and apathy are also common following stroke or TBI and should be considered during program design and implementation.
Want to know more? You can learn more about training other Special Populations in the Certified Personal Fitness Trainer Course.