This article was originally published in Issue 13 of Personal Trainer Magazine. You can download the newest issue and all past issues here.
Exercise immunology is the emerging field of how exercise affects the immune system, with most of the research having been done in the past 25 years. With a global pandemic that has dramatically reshaped our lives, it is essential for fitness professionals to understand the basics of the immune system. Well-educated trainers should train and educate their clients in such a way as to strengthen and not compromise their immune system. While this does not guarantee that their client does not get sick, proper diet and exercise are essential to optimize an individual’s defenses.
The immune system is incredibly complex, and this article is intended to introduce some basic concepts pertaining to exercise and one’s susceptibility to infections.
Humans are continually exposed to many infectious agents such as viruses, bacteria, fungi, protozoans, and parasites, all of which could make one ill. The immune system’s job is first to prevent the entry of these infectious agents and second, if they can get past our natural barriers, to neutralize the threat.
Here Are Some Supplements That Can Boost Your Immunity
The two main branches of the immune system are innate immunity and adaptive immunity. Innate immunity (also
known as “non-specific”) protects the body without distinguishing one threat from another. This includes barriers such as epithelia which lines and covers the body (e.g., the epidermis of the skin, mucous membranes of the respiratory, digestive, and reproductive tracts), and specialized cells (phagocytes, natural killer cells), proteins (interferon, complement) and physiological processes (fever and inflammation).
Adaptive immunity (also known as “acquired” or “specific” immunity) will respond to a specific infection such as a virus (e.g., the flu, COVID-19) and make specialized immune cells designed to neutralize and kill that specific virus. There are both cellular and humoral components. Cell-mediated immunity consists of specialized lymphocytes known as T-cells, which kill already infected cells. Humoral immunity (“humoral” meaning relating to bodily fluids) consists of B-lymphocytes that create specialized proteins known as antibodies found in the blood plasma.
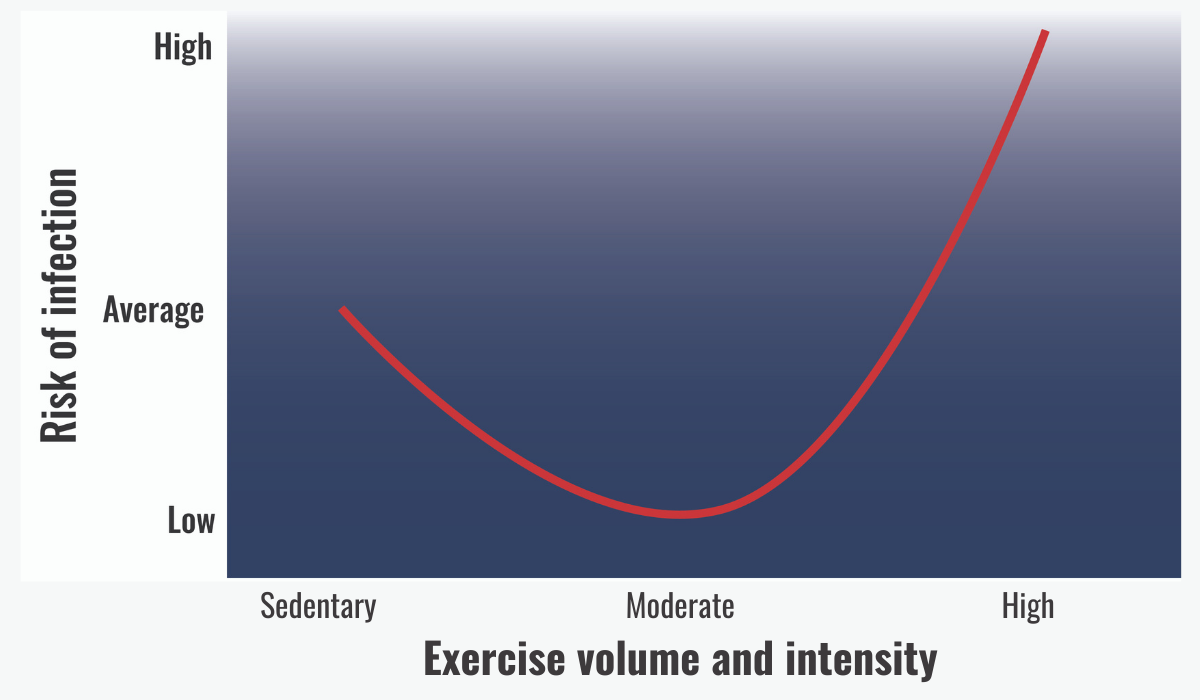
The impact that exercise will have on the immune system is dependent on the exercise intensity and volume. For example, one of the most studied areas in exercise immunology is the effect of exercise on upper respiratory tract infections (URTIs). In the case of URTIs, exercise can have positive and negative effects. Individuals who participate in regular moderate exercise have been found to be at a lower risk of URTIs. However, the risk of a URTI increases in individuals who engage in intense and/or long-duration exercise. The risk of infection in these high-intensity athletes can be higher than that of a sedentary individual. This is represented by a J-shaped curve.
It is thought that regular 20–40 min of exercise at 40–60% VO2 max is sufficient to reduce the risk of URTI by up to 67%.
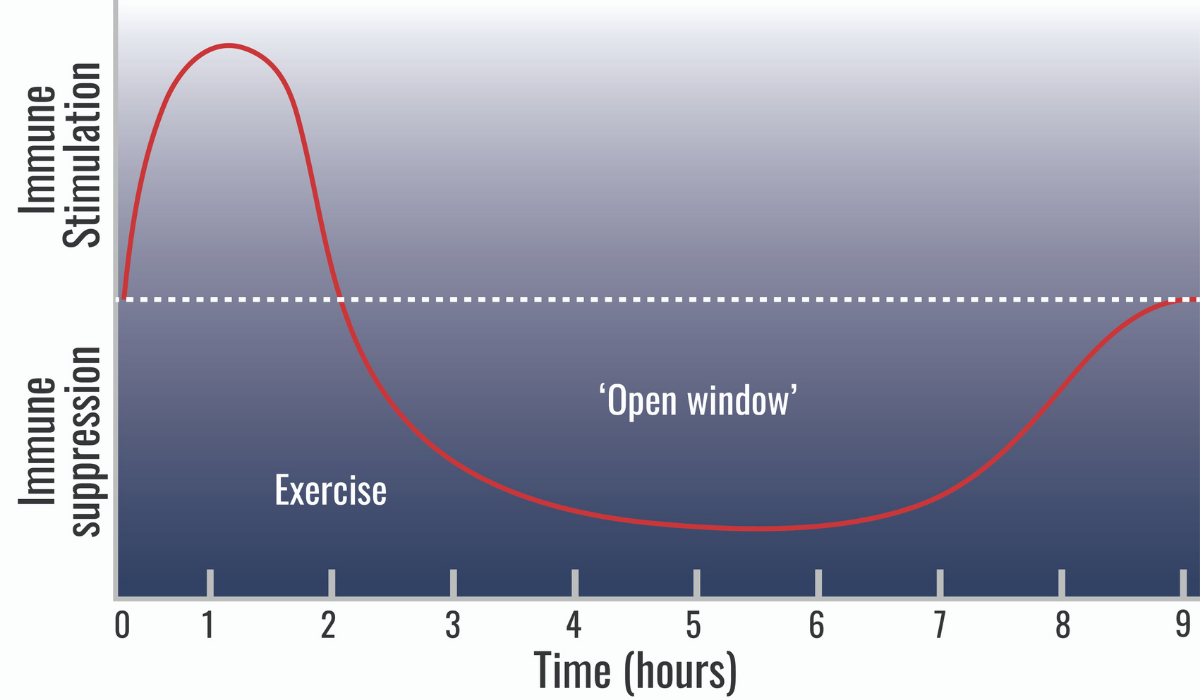
Heavy intense exercise can transiently suppress immune function up to three hours post-exercise. Many studies demonstrate that after an intense bout of exercise, the humoral branch of adaptive immunity and, specifically, antibody production is transiently suppressed at least one-hour post-exercise. For example, one study was performed on eight well-trained cyclists who exercised for two hours at 75% of their VO2 max. In this study, antibody production dropped 50-65% for one hour after exercise.
Here Are Some Supplements That Can Boost Your Immunity
Other studies have shown similar decreases in the cellular branch of the adaptive immune system. Specifically, prolonged exercise (i.e., greater than 90 minutes) has a temporary depressive effect on the immune system. This is seen by a decrease in levels of B-cells and T-cells as well as a decrease in natural killer cell activity. This is common for athletes such as marathon runners, where immunosuppression would last for up to six hours.
Taking together the suppression in both humoral and cellular immunity immediately post-exercise has lead to the “Open Window Theory”. This theory states that your immune system is transitorily suppressed for several hours after an intense bout of exercise. This gives any opportunistic bacterial or virus the chance to get a foothold leading to infection.
possible mechanisms for this temporary suppression in immune function after exercise is the elevation of several stress hormones. These include the adrenal hormones of cortisol (secreted by the adrenal cortex), epinephrine, and norepinephrine (both secreted by the adrenal medulla), which are known to be immunosuppressive. Additionally, an increase in body temperature as occurs during exercise may also play a role in immunosuppression. In addition to other common factors such as lack of sleep, mental stress, and increased exposure to pathogens, an athlete’s susceptibility to infection can increase.
In summary, multiple variables can affect an individual’s immune system. Moderate exercise has been shown to boost the immune system, while high-intensity/long-duration exercise has a temporary depressive effect. As fitness professionals, we must be aware of the benefits and risks of exercise and how to program appropriately to optimize our clients’ health.
Here Are Some Supplements That Can Boost Your Immunity
Getting Started
Check out what it takes to start a career in personal fitness training. This is your most affordable and fastest way to become a highly qualified personal trainer.
Is your recertification coming up? Learn more about earning your CEU credits. You can find the full list of CEU courses here.
There is always something exciting about earning a new training or coaching certification and applying that new knowledge of how you train your clients. This also helps you hit the reset button.
NESTA and Spencer Institute coaching programs are open to anyone with a desire to learn and help others. There are no prerequisites.
That’s it for now.
Take action!
PS: Click here to see many helpful business/career resources